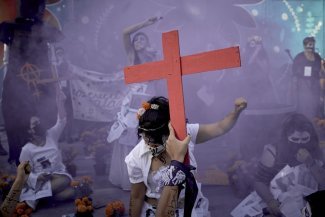"I love caring for my patients. It’s a great privilege to have their trust and I see my colleagues – from consultants, cleaners, nurses, allied healthcare workers to admin staff – work extremely hard everyday to honour the trust patients have put in us,” says Dr Sarah Alhulail, a trainee general practitioner (GP).
“But we need to be able to continue functioning safely and effectively to provide the care our patients deserve, and this government’s policies make this more difficult everyday."
Sarah is one of nearly 50,000 junior doctors in England who are currently fighting a new contract proposed by Prime Minister David Cameron’s Conservative government.
In February, Health Secretary Jeremy Hunt announced that the government will be imposing the contract despite ongoing industrial action. This move has led to the escalation of strike action that was approved by 98 per cent of junior doctors in a ballot late last year.
Following walkouts in January, February and March, junior doctors across England will be staging two 48-hour strikes in April, starting on 6 April and 26 April. The latter will involve a full withdrawal of labour between 8am and 5pm, including accident & emergency as well as intensive care.
On announcement of the escalation, Dr Johann Malawana, British Medical Association junior doctor committee chair said: “No junior doctor wants to take this action but the government has left us with no choice. In refusing to lift the imposition and listen to junior doctors’ outstanding concerns, the government will bear direct responsibility for the first full walkout of doctors in this country.”
Alhulail fully supports this decision. “Imposition does not have any place in a democratic society when you are dealing with experts and professionals who are saying ‘No.’"
The new contract: "not safe, not fair"
The disputed contract is part of the Conservative Party’s healthcare reform agenda, which is intended to lead to a ‘seven-day National Health Service (NHS)’.
To facilitate this, the new junior doctors’ contract would extend core working hours to cover Saturdays 07.00 to 19.00 as well as weekdays until 22.00. To compensate for the loss of extra pay for unsociable hours, basic pay would be increased.
But industry professionals say the new contract is neither safe nor fair. They are calling for more resources for the overstretched and underfunded NHS.
"We think the contract fundamentally goes against the long-term delivery of patient care and is unfair on junior doctors, many of who work the most unsociable hours," a BMA spokesperson tells Equal Times.
Doctors at the start of their careers are junior, although this can mean nearly a decade of experience. They comprise the majority of the NHS’ weekend workforce, and many find it impossible to combine childcare responsibilities or keep up with the required training with such irregular shifts.
"Every day we have gaps in the rota, and trust grades [doctors who do not take further training] and nurses filling those gaps in some areas. Every year, training posts are removed," says Dr Dominic Pimenta, a core medical trainee from London.
The BMA has provided the Health Secretary with a cost-neutral alternative they consider fairer. They are calling for the government to return to negotiations.
Strong public support
A poll for the BBC following the latest strike in March found two-thirds of the public support the junior doctors.
Trainee GP Dr Eimi Howse has been "overwhelmed" by the support.
"On social media and out on the picket line, ordinary people have been approaching me and my colleagues with support. It has galvanised the inter-professional solidarity amongst different staff groups in the hospital, too," she says, describing nurses and consultants bringing tea and home-baked treats to the picket lines.
When asked whether the dispute has politicised the medical profession, Howse says it has.
"Doctors tend to be a middle of the road bunch. They work hard and keep their heads down. But since this dispute began, the willingness of the government to push through their unsafe and unevidenced contract for the purposes of their own corporate interests has opened this generation of doctors’ eyes to the injustice of the current Conservative agenda."
A BMA spokesperson is more cautious in his assessment. "I don’t think it is right to say ‘politicised’: it is a contractual dispute. But it has affected the morale of junior doctors around the country so it is definitely having a broader impact."
"Many of us do feel really quite down trodden about the whole thing. The uncertainty about what sort of rota we will be working and how much we will be paid come August is unnerving," Howse explains. She asserts that while she has no plans to abandon the NHS, she doesn’t want to work under the new contract, either.
"I’m determined to stay and fight for an NHS that is publicly funded, publicly provided and free at the point of care."
On the road to privatisation
Alhulail says the NHS’s "existence makes the case for publicly provided healthcare all over the world."
The Kuwaiti-Egyptian does not take the NHS for granted and campaigned against privatisation prior to the current dispute "because I know what the alternative experience is like, in an inadequate public system or an exploitative private system."
In 2012, the UK government passed the Health and Social Care Act. Many of the changes apply to England only; the NHS in Scotland, Wales and Northern Ireland is structured differently.
The Act lays the foundations for privatisation by outsourcing services such as security, pharmacy or IT to the private sector; creating market mechanisms for the distribution of funding within the NHS; and converting hospitals into Foundation Trusts that can raise funding through charging private patients.
Campaigners worry that in the long term, this will undermine the public provision of healthcare.
Unite the Union estimates that the value of NHS contracts in the private market will reach £20 billion in just a few years – a lucrative emerging market for big multinationals such as Serco, Virgin Care and Circle.
Under the 2012 Act, GPs are responsible for commissioning services to private providers. Many of them do not want the responsibility and are therefore likely to outsource the commissioning process itself to consulting firms such as Deloitte, McKinsey or PriceWaterhouseCoopers, according to Unite’s Save Our NHS campaign.
For Pimenta, the future of NHS looks bleak. "This is already an acute crisis, without the imposition and retention pressures created by this contract. The whole system is slowly falling over, and that’s what it feels like inside. I know many friends who have quit – relatively senior doctors with only a few years left of training." He has effectively left, too: he is taking no further training and is assessing his career options. "It is deeply saddening."
Howse says the workforce is reaching a "breaking point." But for her there is still room for optimism. "The dispute has made us stronger together and that really makes the working environment more cohesive and positive. Hopefully we can keep that up."