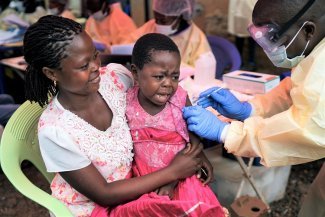
Patients and health workers in a dialysis unit in Idlib, funded by the NGO Mehad (formerly UOSSM), 27 February 2023.
In the corridors of the Avicenna Dialysis Centre in the city of Idlib, north-west Syria, the comings and goings are endless. In one room, under the watchful eye of nurses, a constant flow of patients receive dialysis sessions, lined up on around ten beds and covered with thick blankets. The centre is open 24 hours a day and is one of eight dialysis units in Idlib province, one of the Syrian regions hardest hit by the 7.8 magnitude earthquake that struck Turkey and Syria on 6 February 2023, claiming over 50,000 lives. Around 4,500 of the deaths were registered in Syria, where over 8,500 people were injured.
“Even before the earthquake, we were not able to provide sufficient dialysis sessions for our patients,” says Dr Taher Abd al-Baqi, who works at the centre. “For the past month, we have been totally under-capacitated, and the patients keep coming. We expect to perform 1,800 to 2,000 dialysis sessions a month. The waiting lists are getting longer and we don’t have enough equipment,” he explains.
According to figures compiled by the World Health Organization (WHO) in the third quarter of 2022, Idlib province, which is home to 3.2 million people (including 1.4 million displaced persons living in camps), had only 36 haemodialysis machines. The urgent need for dialysis has been heightened by ‘crush syndrome’, which has affected hundreds of people after the earthquake, including children. “When limbs are compressed for many hours, the blood flow is cut off, leading to severe kidney damage and heart problems. Some children had to be amputated, when they could have been saved if they had been rescued earlier,” says Dr Fayez Jarad, a paediatrician at the Avicenna Children’s Hospital funded by the Syrian American Medical Society (SAMS), in Idlib, which receives its young patients on small, rudimentary wooden beds. “Despite their outstanding responsiveness, the rescuers did not have heavy equipment to act in the crucial 72-hour period after the earthquake.”
A health system on the brink of exhaustion
The earthquake was the final blow for an already overstretched health system in Idlib province, exhausted by ten years of war, bombing, and the recent outbreaks of coronavirus and cholera. Out of just over 200 health structures in Idlib, nearly 50 were damaged by the earthquake. And since 2012, according to Physicians for Human Rights, 142 health facilities in the region have been shelled by the parties to the conflict, the vast majority by the Syrian regime and its Russian ally. Even before the war, the Idlib governorate was largely neglected by the central government and health services were poorly resourced.
One of the major problems faced by medical staff is the lack of equipment. According to the WHO study cited above, by the end of 2022, there were 64 X-ray machines, five CT scanners and only one MRI machine in north-west Syria. “We have only one CT scanner in Bab al-Hawa hospital, the largest in north-west Syria,” warns Dr Osama Salloum, a surgeon at this hospital on the border with Turkey.
“The anaesthetic equipment in our operating theatres is obsolete, and there is a huge shortage of neonatal incubators, while the earthquake has led to many premature births.
Before the earthquake, a degree of pressure could be taken off by sending 20 to 30 critical patients each month to hospitals in southern Turkey, in Antioch, Iskenderun or Gaziantep. This is no longer possible. “These hospitals have been heavily damaged, and priority is given to patients in Turkey. Since the earthquake, it hasn’t been possible to send any patients across the border,” says Salloum. As there is no radiotherapy equipment in Idlib province, the lives of hundreds of cancer patients are also at risk. “There’s nothing they can do but wait for death,” says the surgeon.
The supply of medicines has also been disrupted for several weeks, as many of the pharmaceutical factories in southern Turkey were partially destroyed. It was not until 11 February, five days after the disaster, that seven WHO trucks crossed the Turkish-Syrian border. In this region of Syria, where more than 90 per cent of the population depends on humanitarian aid, only 26 per cent of its medical needs were covered in 2022.
International aid has been arriving more slowly in the region since 2020, when the Russians used their veto at the UN to limit cross-border aid to a single crossing point, Bab al-Hawa, as opposed to the previous four. The use of the border crossing now has to be renewed every six months by the UN. The next deadline is 10 July.
Humanitarian aid is hard to come by
After the earthquake, the Syrian regime finally agreed to open two more border crossings for three months: Bab al-Salam and Al Ra’ee, following tough negotiations with the WHO. “If the Bab al-Hawa crossing is not renewed this summer, humanitarian aid to northern Syria could fall by 50 per cent, with dramatic consequences. The aid that arrives from areas controlled by the regime covers less than five per cent of the needs,” says Dr Zaher Sahloul, president of the US NGO MedGlobal, which provides support for hospitals in the Idlib region.
The Syrian jihadist group Hay’at Tahrir al-Sham (HTS), which has been in control of the Idlib governorate since 2018, refuses to let in aid from areas controlled by the regime, for fear of having to rely on it in the future. And although there are trade routes between Turkey and northern Syria, if medicines were to pass through there, humanitarian trucks could be stuck for days at the border and taxed by the HTS group. They could also be bombed by the Russian air force.
Over the past three years, international aid has also decreased significantly. Only 48 per cent of the funds pledged by international donors were disbursed in 2022. And cross-border aid to north-west Syria in 2022 represented only 12 per cent of the humanitarian response in the country.
“Many donors withdrew following the takeover of the HTS and then, in 2021, redirected their funds to Ukraine,” says Dr Abdulkarim Ekzayez, an epidemiologist at King’s College London who practised in Syria until 2016. According to the doctor, the jihadist group does not intervene in the management of humanitarian aid.
“The National Salvation Government set up by HTS has a health minister, but he has very limited resources and powers. The coordination of medical aid with the UN and local NGOs is managed by the Idlib Health Directorate, which brings together doctors from the region, is not politicised and has legitimacy on the ground,” explains Ekzayez, also a co-investigator with R4HSSS, a British research programme in Syria. The Health Directorate, which grew out of local coordination committees after the Syrian revolution, was officially established in 2015. It has conducted various vaccination campaigns in the region, against polio, coronavirus, and on 7 March, it initiated a vaccination against cholera, targeting 1.7 million people. “As regards the HTS, we are used to dealing with it, the situation remains acceptable, the bureaucracy is elastic, it depends on the circumstances and the urgency,” says Dr Ahmad Jamal al-Arraj, a doctor in a mobile clinic of Médecins Sans Frontières/Doctors Without Borders (MSF).
Lack of specialist doctors and depression among carers
The Idlib region also lacks human resources. The number of health workers remains “acceptable” in the Idlib governorate, with 11.3 health workers per 10,000 inhabitants, according to the WHO, while the international standard is 22 health professionals per 10,000 inhabitants. But what is most lacking are specialists. “Everything is in short supply: anaesthetists, resuscitators, neurosurgeons, orthopaedic surgeons, oncologists, etc.,” says Dr Ziad Alissa, co-founder of the NGO Mehad (formerly UOSSM), which has trained 30,000 doctors in the region since 2013, first in war medicine, then in other specialisations.
There are also only a handful of psychologists and psychiatrists in the province, although the need is immense. “We see a lot of post-traumatic shock in children, anxiety in men, and depression in both sexes. These disorders are often not people’s first concern, but the longer they are left untreated, the worse they get,” says Dr Ahmad al-Abda, one of the few psychologists in Idlib.
New doctors continue to be trained at the University of Idlib, or at private institutions in the region, but the level is not always up to scratch. “They lack practice, and sometimes they add to the pressures on the health system rather than relieving them,” says Salloum, from Bab al-Hawa hospital.
There are no more foreign doctors in the region, but foreign medical NGOs such as SEMA, Mehad or SAMS come for a few weeks a year to train practitioners. And a diaspora organisation, the Syrian Board of Medical Specialities (SBOMS), has been offering specialised training on the ground and online since 2016. “The training programme is supervised by 23 scientific committees; it conducts exams and grants certificates to doctors. Three cohorts of doctors have been trained since 2019,” explains Ekzayez.
The earthquake could lead to an exodus of new doctors, especially those working in the hospitals on the border. Their turnover was already quite high before the earthquake. “Most of the doctors in Bab al-Hawa live in border cities in Turkey and travel back and forth to Syria every week.
“They have been very badly hit by the earthquake. Some died, others were injured or lost family members. I have seen colleagues crying while performing surgery. And some doctors still haven’t come back,” says Salloum.
The deterioration in health professionals’ mental health is worrying, he warns. “Before the earthquake, over 70 health workers in Bab al-Hawa were already suffering from depression and burnout,” he says. In 2017, the WHO trained non-specialist doctors in psychological support, but not enough to meet the huge demand. “To cope with a very difficult everyday life, doctors tend not to take antidepressants, which are taboo in Syria, but develop addictions to various drugs: crystal meth, Captagon, or even tramadol in high doses. According to the Idlib Health Directorate, more than 15 health workers have died in recent years from overdoses,” says Sahloul.
Despite facing one disaster after the next, most of Idlib’s doctors are determined to stay. With a full white beard and a stethoscope hanging around his neck, Abd al-Baqi is finishing his rounds at the Idlib Dialysis Centre and is determined to keep his spirits up. He says he could have left as soon as the war started for Saudi Arabia, where he did his specialisation, but he decided not to go. “It is not rational to stay here, I know my children would have had a better education and more opportunities abroad. But this is my destiny, I can’t abandon my people. My consolation is that I am on the path to freedom, humanity and justice.”