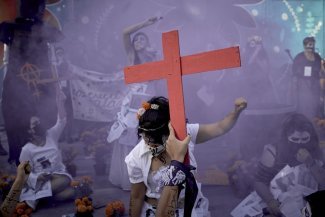Genyo genomics unit in Granada, one of the most advanced oncological research centres in Spain.
The fact that cancer is a silent illness is something that was already known during the times of Hippocrates. Despite its skill at camouflaging itself, we now know that it leaves some loose ends. When a tumour cell grows and spreads to other tissue, or dies, it leaves part of its genetic information in the bloodstream. And that is a fatal blunder. Because it leaves the body full of clues.
Dr Luis Javier Martínez and his team are tasked with finding them. They examine blood in search of intruder cells at the genomics unit of the Genyo research centre in Granada, Spain. It is thanks to these cells that they are able to discover what the tumour is like, whether it is growing or shrinking, whether it is responding to the medication or if the dose needs to be changed. All of this, without having to do a puncture or a biopsy: a simple blood test is all that is needed.
“Taking a solid biopsy is a very invasive procedure and, depending on where the tumour is located, is not always an option. That is what makes this new technique – the liquid biopsy – so revolutionary, explains Rosario Sánchez, chief researcher at Genyo.
Our genes are the Rosetta Stone of this medicine of the future that is being tested, right now, in laboratories like this one, where test tubes stand side by side with huge computer processors. Technological development is facilitating ever more precise techniques. And it is doing so at unimaginable speed. Whereas in 2003 it took 37 laboratories throughout the world to decipher the human genome, and it took them almost 13 years, “we are now able to sequence a genome here within a day,” says Martínez, head of the unit.
Thanks to this information, we now know which genes make us predisposed to which illnesses, but we have also discovered that we do not all respond the same to the same treatment; that the same antibiotic for the same infection may or may not work for you, depending on your genetic makeup.
New precision or personalised medicine is based on that principle. Rather than blindly attacking a disease, genetic clues, or biomarkers, are sought, so that each individual can be given the drug that best suits them. “The idea is to group patients according to their genetic profile. That way we can also prevent diseases, make a better early diagnosis,” says Sánchez.
The first test line is oncology, but it will soon be extended to diabetes or Parkinson’s. The idea is that, in a not too distant future, doctors will not only be handling our medical records but all the information about our genome. They will be able to prescribe the right treatment from the very outset, and will know what illnesses we risk contracting, no matter how silent they are.
A universal medical revolution?
Around 30 per cent of the new medicines approved in 2017 were already based on genetic information – directed at mutations or specific proteins in our DNA. The question is, as well as being more precise, will the medicine of the future also be universal, or will this revolutionary healthcare be the reserve of a small part of the global population?
The World Economic Forum itself has already expressed its concerns: “Precision medicine requires sophisticated screening technologies not available in many parts of the world. There is even potential for precision medicine to increase inequality in medical care and wellbeing between countries and the socioeconomic groups within them.”
These fears are well founded, bearing in mind that two billion people – a third of the global population – does not currently have access to even the most basic medicines.
Spain’s national pharmaceutical industry association Farmaindustria acknowledges that these new drugs “will not be used by hundreds of thousands of patients but much less, which means the price will be higher.” Especially given that “the research and development process is long and costly”. It does, however, point out that new ways of covering the costs should be found.
“Precision medicine may mean an initial investment, but it will undoubtedly lead to savings in the long run,” says Consuelo Martín de Dios, managing director of the Roche Institute Foundation. The savings will come from reducing the amount of unnecessary medication and tests, which will in turn reduce the number of patients needing to be admitted to hospital. This precision will prove useful in societies that are growing increasingly older and suffering from more ailments.
Over and above the costs, the tasks currently at hand are the creation of a regulatory framework, such as those already introduced in the United Kingdom or France, the training of health professionals and the improvement of the infrastructures needed to store and analyse the huge amount of data contained in our genes.
To give us an idea, each human genome is the equivalent of around 10 million tweets. “Genome sequencing generates more data than astronomy. That’s where the hitch lies. How are we going to manage to analyse all that data?” asks bioinformatician Gonzalo Claros.
And there are other issues. What is going to happen to all the data about our genetic profile, and in whose hands could it end up? And, above all, will we be able to cope with knowing so much about ourselves? That is the debate we need to have.
Between myth and phobia
“I was operated on 30 years ago and things have moved on tremendously since then. In the past, you would be told you had breast cancer and that’s it. There was one and the same treatment for everyone. Now each tumour has a name,” says Paqui Aguilar, president of ASAMMA, an association for women operated on for breast cancer. As she points out, the progress in personalised medicine is already improving the lives of many women.
There is a test for patients with a certain genomic profile known as HER2-enriched. A blood test is now all that is needed to know whether a patient will have to undergo chemotherapy or not. “Imagine what that patient is spared. Chemotherapy is very aggressive,” insists Aguilar.
The test is used for a specific category of women – 20 per cent of those with breast cancer – and always on the doctor’s orders. But what would happen if there were no limits, if anyone could take a genetic test to see what illnesses they have or may develop? That is what is already happening in the United States.
In 2017, the US government authorised the direct sale of genetic testing kits to consumers. No illness or doctor’s prescription is required. They are sold online and can be bought for between US$60 and US$200 from sites such as Amazon. Analysis of a saliva sample is all that is needed to know whether you are likely to have cellulite in the future or to discover your ancestors’ roots. The implications are potentially dangerous.
Genetic information alone, without adequate medical interpretation or guidance, is not conclusive. It is too much complex data to read and digest. “We have created a myth around genetics. This obsession with testing is an illustration of our lack of health culture,” says Fernando Bandrés, president of the inter-university education forum for biomedical ethics, Aula Interuniversitaria de Biomedicina, Ética y Derechos Humanos.
The best example is known as the “Jolie effect”. When actress Angelina Jolie announced she was having a preventive double mastectomy for fear of inheriting breast cancer, the demand for genetic tests shot up by 40 per cent.
“We need to be cautious, we are going to have a great deal of information but we first need to learn how we are going to use it,” says Mariano de la Figuera, from SEMERGEN, the Spanish society of general practitioners.
It is the family doctors that are going to be the first to have to deal with this obsession with knowing everything. “What is going to happen when we start to make early diagnoses of incurable diseases, such as Alzheimer’s? Knowing that you are going to suffer from an incurable disease does nothing to help anyone,” he warns.
Alongside those creating a myth around genetics are those who fear it. Warned by dozens of science fiction films, many fear that their biological data will fall into the hands of companies and insurers, which will end up practising genetic discrimination, as the 1997 film Gattaca predicts.
“All progress involves a risk and the risk lies in how that information can be misused, but that shouldn’t hold us back. The more data we have, the better the predictions will be,” argues bioinformatician Gonzalo Claros.
And this is only the beginning. How many misgivings can we expect when the day comes that researchers can not only read genes but also modify them? “A very profound change is taking place, like the Renaissance, the difference is that now it is very fast. At the same pace as the new technologies astonish us, we have to generate a debate,” says Bandrés.
To start with, we must not forget the fact that we are not simply genes. We are also the environment in which we live and the lifestyle we lead. As Doctor Mariano de la Figuera underlines, no matter how much we discover from DNA, medicine continues to be an inexact science and “the only thing that is 100 per cent genetically determined is that everything that is born, dies”.